Apparently, it’s not old age.
Two weeks ago, I reported on my aches and pains and my oncologist’s suggestion that it can likely be ascribed to “getting older.” Maybe some of it can, but some of it certainly can not.
Two Saturdays ago I woke up with more-than-usual pain in my lower-right back and, after a raucous internal debate, decided the time had come to go to the hospital. I discussed with Tammy, and she came to the decision that the best course of action would be to call an ambulance. A quick call to Magen David Adom and, minutes later, a trio of volunteers shows up at our door, ready to whisk me to Hadassah Ein Kerem, where I get my usual care.
The volunteers were great. They were patient, helped me down the stairs (no elevator) and  into the van, and the young guy who was driving took care as best he could to avoid bumps and dips in the road. No need for lights and sirens; avoiding extra pain due to unnecessary jarring was the name of the game.
into the van, and the young guy who was driving took care as best he could to avoid bumps and dips in the road. No need for lights and sirens; avoiding extra pain due to unnecessary jarring was the name of the game.
We were brought right in, I was immediately placed in a bed and in (what seemed to me, at least) moments, I was being attended to by ER doctors and nurses, with someone from oncology on the way.
The immediate concern was to determine the source of pain, most likely: (1) my liver stent which you will remember was inserted in March of this year, (2) an infection, possibly due to the stent or something else, likely my right kidney, (3) something else.
I had brought along all of my meds that I take on a regular basis, which made answering the question of “What medications are you currently taking?” a whole lot easier to answer. And, when I was asked if I wanted morphine in addition to what I already take, the answer was a quick, “Heck, yeah!”
There was no question I needed to be admitted and tests administered, starting with blood cultures and an ultrasound. The only challenge was there were no available beds in oncology (Yes; it’s becoming an epidemic.), but a place was found in the new building, on the Plastics/Ear Nose Throat floor (Why are they together?) and I was moved in what seemed like no time at all (thanks to morphine?) to the seventh floor.
So far, so good, right? Yeah, that should have raised an alarm.
We spent the rest of the afternoon listening to my roommate snore and having pain meds administered as often as possible. But no ultrasound.
Sunday was spent listening to my roommate snore and having pain meds administered as often as possible, until midday, when we saw the oncologist who was responsible for my care, at that point. She was somewhat surprised I hadn’t had the ultrasound yet and when she spoke to the nurse, she was told it was never ordered. She was slightly perturbed and said, “It’s ABC, of course he needs an ultrasound!”
“But no one ordered it.”
And so, it was ordered. The oncologist then offered a piece of advice: sometimes it’s helpful if a family member goes down to politely ask if their loved one can, you know, be seen in a timely manner. So Tammy did that and was told by the receptionist that she had “no clue” when I would be called. About an hour later, Tammy went back and this time, the receptionist was a bit nicer and said they were ready for me.
As I’m laying on the table, the technician starts asking me useful and helpful questions like, “Didn’t anyone tell you to fast before this?” and “How come you don’t have a previous ultrasound for comparison purposes?” and “How am I supposed to tell what I’m looking at?”
With that great experience behind me, it was back to my room for more waiting and snoring (not mine) and pain meds.
Monday morning comes and a new oncologist has taken over. He ordered a CT and told me that I’d have to wait a while to have it done, likely “after 5pm” when things calm down. So, I assume the good news here is that I’m not an emergency case and that it has been determined I could wait.
And wait I did. With increasing pain. So much so that every breath I drew caused stabbing pain on my right side.
At 5:00 a.m. Tuesday I asked the nurse why I need to wait so long for my CT and she understandably had no idea. She offered to call the CT receptionist at 7:45, as that’s when the counter opens. So I texted Tammy and asked her to be at the hospital by 7:30 to go herself to the CT desk. Which she did and had the following exchange as she crouched to engage the receptionist who was hiding behind a closed window shade with about an inch of room:
“Can you tell me when my husband’s CT will be?”
“Uhghh-mnn,” delivered with a shrug, as in “How should I know?”
“My husband is lying in bed, suffering, and waiting for the CT so the doctors can know how to help him. What can you do to help us?”
No response, but she did look at the computer, after which she replies, in intelligible Hebrew, that she will call for someone to get me. Which she did because as soon as Tammy got back to my room, someone was there to take me down to the CT. Here’s the best part: know how long the CT itself took? About 90 seconds. That’s right. There was apparently no time the day before for a 90-second CT. (I seriously don’t know what how patients who have no one to advocate for them get by.)
Back in my room by 8:30, the oncologist came by shortly thereafter and said that he saw the images and this is clearly a case for urology as the issue is with my kidney – hydronephrosis – inflammation of the kidney. (Liver functions all came back OK.) Shortly after 9:00, the urologist stopped in to introduce himself and to explain what would happen next.
Let me tell you, of all the doctors I’ve met in the past five years, this guy has possibly the best bedside manner. He was calm, patient, willing to explain things several times and, when I was brought in for the procedure (details in a minute), he insisted on first sitting with us to review my ultrasound and CT images to explain in detail what he intended to do.
The hydronephrosis was caused by a blockage in my right ureter, which moves urine from the kidney to the bladder. In all likelihood, the blockage was caused by a tumor and, the 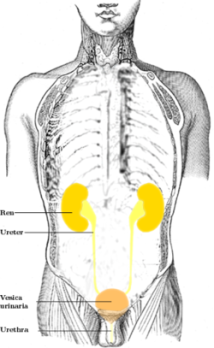 good doctor’s plan was to open the blockage and insert a stent to keep the urine flowing more freely.
good doctor’s plan was to open the blockage and insert a stent to keep the urine flowing more freely.
There are a couple of ways to achieve this. The preferred method is non-surgical and requires inserting a wire and stent directly through the bladder into the ureter. How is this done non-surgically? Well, let me put it delicately and say it involves lots of local anesthetic, a very steady hand and absolute faith in whomever is performing the procedure. A sedative is possible but highly undesirable as it renders the patient unable to follow directions.
Using a portable x-ray machine (don’t know how else to describe it) the doctor saw, once he was in, that things were a bit more complicated than anticipated. (No surprise there, right?) See how the ureter basically goes straight down in the image to the right? Well, not mine. Due to a blockage right near the bladder, the upper portion was S-shaped. So, before being able to insert any stent, the whole thing needed to be straightened out. That’s when the fun began. No local anesthetic up near my kidney, so I felt every manipulation, twist and turn. Several times, he was ready to stop to acquiesce to the second option (involving incisions and drains and more days of pain, I believe), but the colleague assisting with the moveable x-ray kept encouraging the doctor who, I think, was so overcome with guilt for the pain he was causing.
In the end though, it was a success and as soon as I stood up from the table, I felt relief starting. I was able to breathe. Yes, there was urine and blood everywhere and I no control over anything.
But I was able to breathe.
To test whether the kidney would drain, the doctor had injected some dye into my kidney at the end of the procedure and asked me to move around a bit for about 10-15 minutes, emptying my bladder as the urge came. I did and then got back on the table. You should have heard the exclamations of joy from the doctor when he saw that my kidney had completely drained!
So, I was eventually sent back to my room, wearing a diaper, knowing I had very little control over my bladder and enduring intense pain whenever it emptied.
But I was able to breathe.
That evening, I was reminded of something I had almost forgotten: every meal can and should be a Meal of Thanksgiving. After not eating for about 24 hours, I was able to enjoy – not just tolerate – a sandwich Tammy had bought for me. My appetite was returning. I was in less pain.
And I was able to breathe.
The oncologist came by later that afternoon to take more blood for cultures and informed that if everything comes back OK, I could go home, likely in two days. Wouldn’t you know it, but the next day, Wednesday, all was OK, and I was discharged around noon.
I still don’t have complete control of my bladder, and the pain is pretty intense every time I empty it, but at least I can breathe pain-free. I acquired a package of Depends pads so at least I can be out and about with confidence, just like in the commercials!

Holy P…s! What an ordeal!
Sent via BlackBerry from T-Mobile
alan, your positive spin on everything is inspiring.
I’m crying and laughing Alan! I’m glad you’re feeling better. Wishing you a refuah shelaima!
You’ve impressed me on many levels with this post: number one: it’s clearly not all about the parking when you take an ambulance. Number two: glad to hear that your internal organs are forming the shape of an S, one of my clearly beloved initials. Three: that you’re breathing without pain. Four: that you always manage to find the humor in any Situation. Thanks for reminding us that a sandwich is not just a sandwich it’s a lesson inThanksgiving –turkey or otherwise.
So when are you going to be in one of those Depends commercials?
I was looking for a clip on YouTube from Mr Saturday Night, that great Billy Crystal movie, where he does an adult diaper commercial toward the end of his career. Absolutely hysterical, but alas, could not find it.
Reading your posts is a gift. Not just your humor, but your appreciation and perspective for your own matzav gives us all the same for ours. Thank you and a continued refuah shleima!
Wow, Alan! I’m speechless. Refuah shalama. And keep up that incredible strength!
Cheryl
On Sep 4, 2016 11:20 AM, “Its all about the Parking” wrote:
> Alan posted: “Apparently, it’s not old age. Two weeks ago, I reported on > my aches and pains and my oncologist’s suggestion that it can likely be > ascribed to “getting older.” Maybe some of it can, but some of it > certainly can not. Two Saturdays ago I woke up with” >
Thank you Cheryl!
Alan,
You’ve been through the ringer and you still hold your head up high for the next day! You are so brave, hence why you are a Braverman and you are right, depends are nothing compared to breathing! You are not alone, I have to wear them too with my colitis and the only person that knows you’re wearing it is you and maybe Tammy! Glad you are on the road to feeling better!! You are always in my thoughts and prayers!!
Beth
Well, now pretty much everyone knows!
Sounds very good to me! I hope you keep improving!